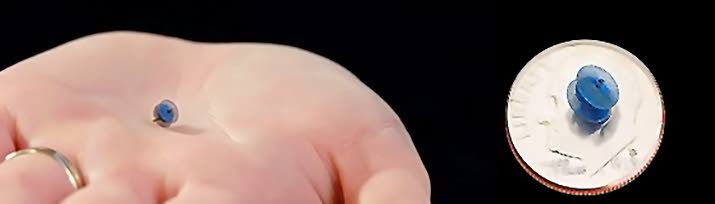
Tiny device with life-saving impact
Loading article...
A groundbreaking advancement in paediatric heart care is transforming how doctors treat one of the most common and potentially serious conditions affecting premature babies. A tiny, minimally invasive device, smaller than a dime, is now helping close dangerous heart defects without the need for surgery.
The condition, known as patent ductus arteriosus (PDA), occurs when a blood vessel connecting the aorta and pulmonary artery fails to close after birth. This vessel, which is essential for foetal circulation, is expected to seal naturally within the first few days of life. However, in premature infants, that closure often does not happen.
PDA is especially common among preterm babies, affecting an estimated 30 to 60 per cent of infants born before 28 weeks of gestation. Globally, with approximately 15 million babies born prematurely each year, this translates into hundreds of thousands of infants at risk of complications linked to the condition.
While some cases resolve naturally, larger openings can place life-threatening strain on a newborn’s heart and lungs, particularly in fragile, low-birth-weight infants.
“If it’s large, especially relative to the patient, it can create a number of problems,” explained Peter Guyon, paediatric and congenital interventional cardiologist at Joe DiMaggio Children’s Hospital in South Florida. “It puts extra stress on the heart and strain on the lungs.”
Medical experts note that untreated PDA in premature infants can lead to serious complications, including respiratory distress, heart failure, poor growth, and an increased risk of chronic lung disease. Studies suggest that significant PDA contributes to higher morbidity rates in neonatal intensive care units (NICUs), particularly among extremely low birth weight infants.
Traditionally, treating PDA in premature babies often required invasive surgery or transporting critically ill newborns to operating rooms designed for larger patients. Both approaches carry substantial risks. Surgical ligation, while effective, has been associated with complications such as infection, vocal cord injury, and longer recovery times.
Now, a new approach is changing that reality.
Physicians can perform the procedure directly at the baby’s bedside in the NICU using a minimally invasive technique. By accessing the heart through a small blood vessel in the leg, doctors guide the tiny device into place, where it expands to seal the opening. Over time, the body naturally heals around it, eliminating the defect without the need for incisions.
“We didn’t always have devices small enough for these tiny babies. Now, we can treat them safely without moving them from the NICU, which is a major advancement,” Dr Guyon said.
This innovation is particularly important, given that premature infants often weigh less than 1,500 grams (3.3 pounds), making them highly vulnerable to stress, temperature changes, and movement. Avoiding transport and surgery significantly reduces these risks.
At Joe DiMaggio Children’s Hospital, specialists are among a select group participating in clinical trials of this next-generation technology, with the goal of expanding its use and establishing it as a new standard of care.
Over the past two years, approximately 30 bedside procedures have been performed using this method, all with successful outcomes and no reported long-term complications. While larger studies are ongoing, early data from similar minimally invasive PDA closure techniques show success rates exceeding 90 per cent, with shorter recovery times, compared to traditional surgery.
“Our surgeons are excellent and can do incredible work. But whenever we can avoid surgery, especially in such vulnerable patients, this offers a safer and highly effective alternative,” he said.
As innovation continues to reshape paediatric medicine, advances in minimally invasive technology are improving survival rates and long-term outcomes for some of the most vulnerable patients. For premature infants facing life-threatening heart conditions, this tiny device represents something far greater than its size suggests – a safer start to life.
keisha.hill@gleanerjm.com